Saint Joe on solid footing
As some EKY hospitals falter, AI and other efficiencies will keep Berea facility strong, according to leadership

CITY HALL – Over the summer, a report issued by policy wonks in North Carolina warned that hundreds of rural hospitals will be at risk of closure once cuts to federal health spending becomes law in 2027.
On that list of 338 rural health facilities scattered across the nation and destined for doom was CHI Saint Joseph Berea.
But CHI Saint Joseph's market president, Matt Grimshaw, told City Council in its second regularly scheduled meeting this month, that Bereans needn't worry because our Saint Joe's is more than ready for the coming storm of federal cuts set to take place 2027 through 2032.
"I was very dismayed with the report getting national attention, Grimshaw said. "It's a very rudimentary analysis of the hospitals across the country, without even looking at market positions or medical performance, or community support. None of those metrics were factored in," Grimshaw said.
'Single payer' approach
According to KFF, a nonpartisan health research nonprofit, the One Big Beautiful Bill Act will cut federal Medicaid by $793 billion while also reducing spending in the ACA Marketplaces ("Obamacare") by $268 billion over the next decade, for a total of 1.04 trillion dollars in cuts, after factoring in the indirect effects on federal revenues.
Here at home, Grimshaw said the health facility on Estill Street does face what he placed at about 75 million dollars in federal cuts, but he said that what the Big Beautiful Bill did was to standardize rates for both Medicaid and Medicare. "We're really moving closer to a single payer mindset now," he said.
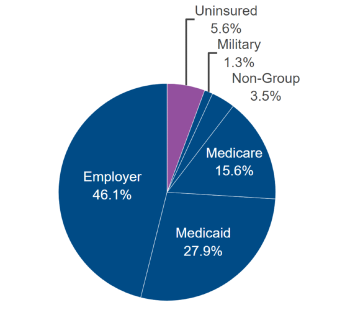
Generally speaking, Medicaid is the federal health payer system for the uninsured, while Medicare is federal health coverage for seniors. Historically, Medicaid rates have been substantially lower than Medicare rates. Both pay healthcare providers at well below commercial rates. Grimshaw said that reimbursements at the Medicare rate means Saint Joe's will still be "viable", and will not run in the negative, despite having less operational cash flow.
However, according to the Centers for Medicaid and Medicare Services, the move to parity between the two federal health payers is only temporary. The new law provides an increase of 2.5% to the fee schedule conversation factor, only from Jan. 1, 2026 - Jan. 1, 2027.
"Yes, it is a cut. Yes, it's real," Grimshaw said. "Yes, it cuts our ability to make some investments but we are doing everything we can now to prepare our ministry and our organization for that five-years-from-now reality."
Grimshaw's reference to "ministry" stems from Saint Joe's being part the nation's largest faith-based, nonprofit health system. CommonSpirit, the parent organization of Saint Joseph Health, was created in 2018 when the Dignity and CHI (Catholic Health Initiative) health systems merged. Saint Joseph's flagship hospital in Lexington was founded by the Sisters of Charity of Nazareth in 1877. What is now called Saint Joseph Berea was founded by Berea College in 1898.
National recognition of services
Grimshaw drew Council's attention to Saint Joe Berea's high rates of patient experience, which are parked at about 95% nationally, and its high levels of medical outcomes which contribute to the hospital's ranking as a Medicare/Medicaid five-star hospital. Grimshaw also said the level of involvement the hospital has in the community is proof the state of the facility is strong.
The hospital has also been recognized by US News & World Report for its clinical distinction in the treatment of colon cancer surgery, heart attack, heart failure, kidney failure and pneumonia.
"If we can't make it here, nobody can make it in the future of healthcare. I give you my deepest word that [closure] isn't even in our thinking, or we wouldn't be here," Grimshaw said.
Instead of closing, the hospital is expanding and recently spent beaucoup bucks on a sleep center, a state-of-the-art nuclear medicine camera, as well as updated imaging technology. The hospital also invested half a million dollars each in a new chiller system to reduce energy use and in a sprinkler fire suppression system. That's all according to John Yanes, president of both Saint Joe campuses in Berea and London, who also addressed Council at the meeting.
The $350,000 nuclear camera has helped turn the Berea facility into a destination hospital, according to Yanes, with referrals from across the region.
"Berea is a small hospital, but a very powerful hospital," Yanes said, crediting the two locations' status within the CommonSpirit Health system. "There's a lot of synergy that comes with being part of a system," Yanes said.
Addressing societal determinants of health
Councilmember Steve Caudill asked Grimshaw whether the hospital plans to emphasize mental health services. Grimshaw said that while no expansion of services is planned, the facility has been investing in Telehealth, which he claimed is the mental health care of "the future of small town services".
"As we talk about community needs, it's nothing really acute, in my mind," Grimshaw said. However, he said that the hospital "does offer real time psych evaluations. A lot of places don't have that, and we do have a seamless transfer protocol."
Grimshaw also threw it back to the City, saying that the underlying causes of mental health crises are due to social determinants of health. "Whether it's housing, food insecurity, all the things that we were just talking about earlier," Grimshaw said, referencing public comment earlier in the meeting, when several residents spoke about their desire to see more collaboration to address societal issues. "How do we resource those community needs together? No one wants to pay for it, right?"
The most pressing need the hospital can address currently, according to Yanes and Grimshaw, is to provide more emergency department care.
Clocking about 16,000 visits annually, Saint Joe Berea's ED has outstripped its capacity, they said. "That space that we are currently using is too small, so we're looking at expanding to a more efficient space to better accommodate patients," Yanes said, noting that many residents without a primary care physician instead use the ED for non-emergent health concerns.
Berea's hospital also serves other health systems such as Baptist Health and UK Health, according to Yanes, offering the region's only "swing bed" program where patients who no longer qualify to stay in the acute care wing but who are also not ready for discharge are given a bed elsewhere in the hospital.
Eastern Kentucky in peril
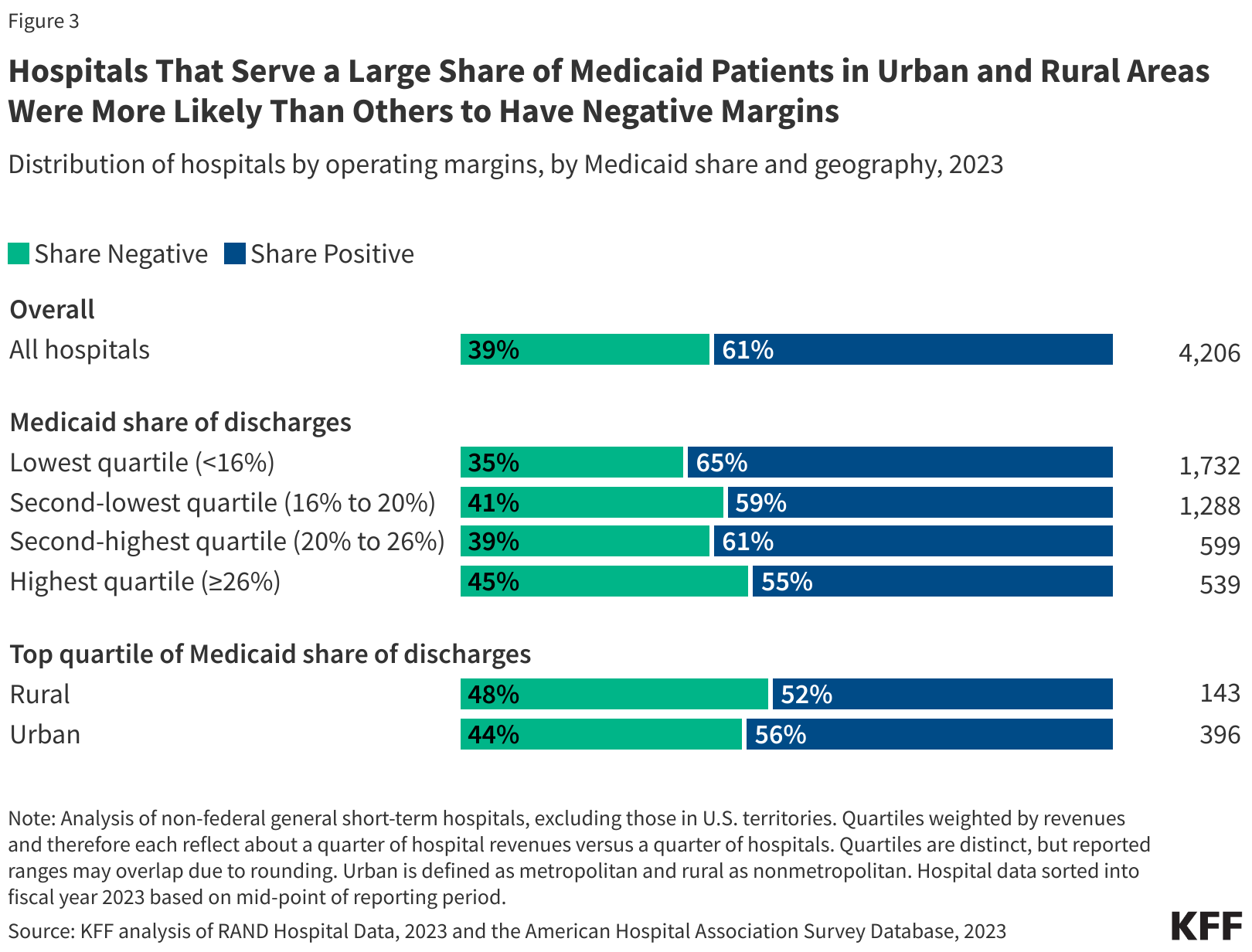
Rumors of the hospital's demise are rooted in a report issued by researchers at the Sheps Center for Health Services Research at the University of North Carolina in Chapel Hill. The report claimed Saint Joe's met two criteria: it is in the top 10% Medicaid payer mix of rural hospitals across the country, and it has experienced three consecutive years of negative total margin.
The report even became the focal point of a letter from Senate Democrats to President Trump in their efforts to keep Medicaid from being severely whacked in the Big Beautiful Bill. They failed, but Saint Joe's leadership told City Council not to panic, because the Shep Center's report did not accurately diagnose the condition of Saint Joe's financial health.
"As we look at communities across the state, we do believe there will be challenges," Grimshaw told Council. "The demographics of Eastern Kentucky are problematic. We are very concerned about the population east of I-75 and south of I-64. All of Appalachia is facing major headwinds, however, we want to be positioned to take care of those patients. We are looking to bring more services to Berea, more service to London, because we believe [patients in] those interstate corridors are going to have to go there for healthcare."
Grimshaw told Council he is concerned that Appalachian Regional Healthcare, which serves much of Eastern Kentucky is the regional system that has the most exposure to the coming cuts because their margins are much thinner than Saint Joseph's.
"They don't have the luxury of being where we are, and we do have conversations about what that means for the patients we share together," Grimshaw told Council.
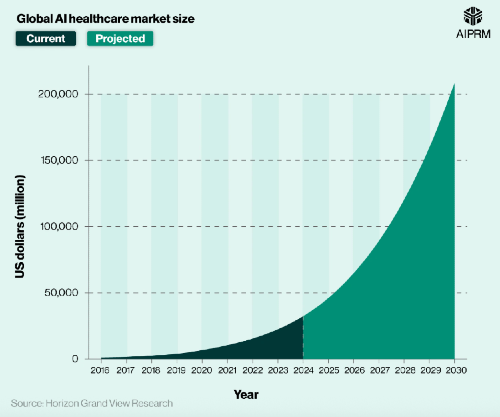
AI, lean management for cost-cutting
Grimshaw said, "I can assure you that as we look across the Kentucky landscape, if our Mt. Sterling hospital and our Berea hospital can't make it, we are looking at a catastrophic failure of healthcare in the state."
In a sidelines interview, The Edge asked Grimshaw how CommonSpirit planned to help both Saint Joe campuses in Berea and London to close the coming funding gap.
"We're leaning in on AI," Grimshaw said. "We are deploying some AI platforms in certain areas to reduce human costs that are deep in the background. Being part of a large system, we have access to resources that others may not."
Grimshaw also said that their system's size allows both Saint Joe's to benefit from "efficiency opportunities", such as Lexington-based call centers and a staff coordination center that each serve multiple hospitals, thus spreading the cost across each facility.
The local Saint Joe facilities also benefit from system-wide performance excellence programs that focus on lean operations for higher quality at lower cost, Grimshaw said in the interview. The programs "quantify all of our objectives with some very clear benchmarks, because we will have to be more efficient in how we care for our populations."
Grimshaw also told The Edge that CommonSpirit will continue to advocate on behalf of Medicaid beneficiaries across the Commonwealth. "Over time, we hope that there will be changes to the legislation, and I expect that there will be," he said.
"Large portions of Kentucky are going to feel the impacts of these cuts," Grimshaw said in the interview. "In Appalachian Kentucky and to the west towards Bowling Green, there are large Medicare and Medicaid populations that we do have concerns about, but we are committed to this community, and to Kentucky. It takes a community, it takes partners, it takes relationships."
November 20, 2025: This story has been updated.
